The endocannabinoid system is an intricate and complicated biological system that is found in all vertebrate species (8). It was discovered in the late 1980s to early 1990s when researchers were trying to understand the effects of cannabis on humans. They realized that the body produces its own cannabinoids, which is why they earned the name endogenous cannabinoids, or endocannabinoids (5, 11). Many functions of the endocannabinoid system are still unknown. What scientists do know is that the main role of this system appears to be maintaining homeostasis, which is the stability of our internal environment. When external factors disrupt the body’s status quo, such as temperature or blood sugar levels, the body needs to internally coordinate to keep everything balanced and functioning (1). The endocannabinoid system sends messages throughout the body to help regulate functions such as sleep, appetite, stress, memory, and mood (9). This complex system consists of three main components: endocannabinoids, receptors, and metabolic enzymes (8).
Endocannabinoids
Endocannabinoids are molecules produced by cells in the body. The two major endocannabinoids are Anandamide (AEA) and 2-Arachidonoylglycerol (2-AG). AEA is a fatty acid neurotransmitter that is also referred to as the bliss molecule, named after the Sanskrit word ‘ananda’ which means ‘bliss.’ This is because it has mood enhancing properties, in addition to helping regulate inflammation and neuron signaling (5). AEA contributes to homeostasis by binding to receptors and encouraging the development of nerve cells in the brain. The development of these new cells is called neurogenesis, and aids learning and memory.
Studies have shown that high levels of AEA cause enhanced mood and reduced fear. High levels of AEA have also been found in people right after completing vigorous exercise, which could explain the ‘endorphin high’ that many athletes experience. Additional research shows that AEA plays a role in ovulation and embryo development. It seems that increased AEA is beneficial for becoming pregnant, and changes in these levels during pregnancy can affect fetal development (5, 8).
2-AG is a compound that is found primarily in the central nervous system. It is the most prevalent endocannabinoid in the human body, and appears to play a bigger role in endocannabinoid signaling than AEA (7). Because of its appearance in immune cells, it is believed to play a role in anti-inflammation through immune suppression (10). It can also be found in maternal milk of humans and cows (8).
Endocannabinoids bind to cannabinoid receptors found throughout the body to signal that help is needed in a particular area (9). Unlike other molecules, they are produced on demand when needed, so the body only creates as much as is required. This differs from classic neurotransmitters which are synthesized in advance and stored until needed (11).
Receptors
Cannabinoid receptors are G protein-coupled receptors (GPCRs). These are proteins found on the surface of cells, in the membrane, and listen to what’s happening in the body. When they detect an issue, they send important information to a molecule in the cell called a G protein, so that the cell can respond accordingly (8). One example of a GPCR is rhodopsin, which responds to light signals detected by rod cells in the eye. The cell will provide an appropriate response to the situation, such as adjusting vision due to dim lighting (12). Cannabinoid receptors are actually one of the most abundant GPCRs (11).
GPCRs are directly involved in human diseases, and therefore, are also the target of many pharmaceutical drugs used to treat those diseases. Because of their role in cell communication, mutations in GPCRs can cause diseases such as retinitis pigmentosa, hypo and hyperthyroidism, nephrogenic diabetes insipidus, and some fertility disorders. Research has found that more than 30 human diseases are caused by GPCR mutations (15). To treat these diseases, many drugs are used that block specific GPCRs. For example, clozapine and olanzapine, which are used to treat psychosis, work by blocking the GPCRs that bind dopamine or serotonin. This interrupts the neural pathways that cause symptoms of schizophrenia. Additionally, some drugs work the opposite way by stimulating GPCR activity. For example, Albuterol activates beta-adrenergic GPCRs, causing airway openings in the lungs to treat asthma (12).
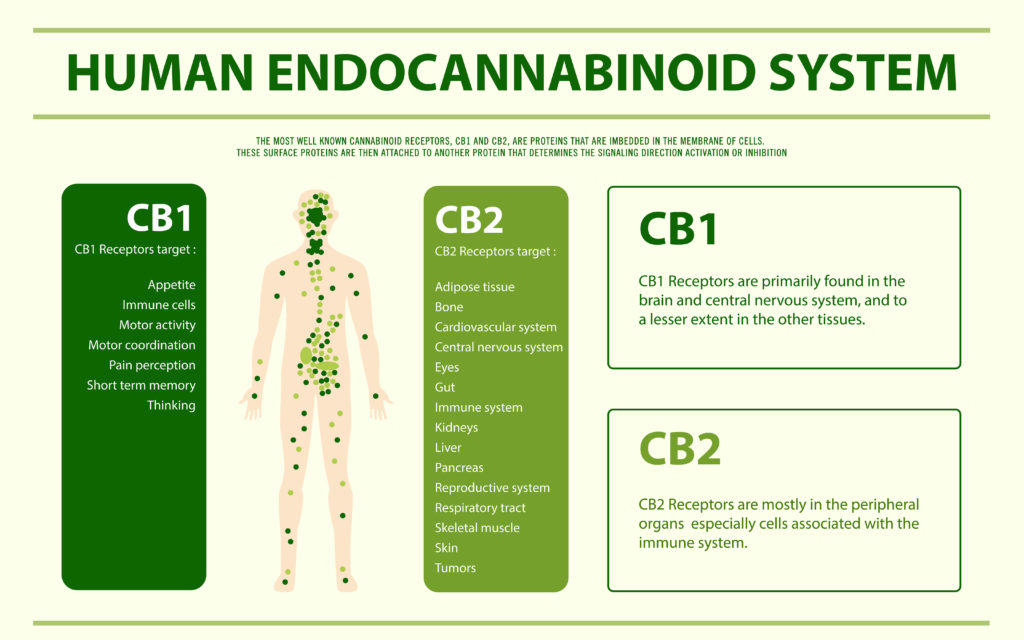
The two main cannabinoid receptors are Cannabinoid receptor type 1 (CB1) and Cannabinoid receptor type 2 (CB2). CB1 receptors are found throughout the central nervous system, with many found inside the brain in areas like the cerebellum, hippocampus, and basal ganglia. They also exist in organs such as the heart, lungs, uterus, and prostate (16). CB2 receptors are located mostly in the immune system. This location coupled with research studies suggests that CB2 receptors have potential therapeutic applications for treating inflammation and allergies (16).
Endocannabinoids bind to these cannabinoid receptors and activate them (8). The effects of this binding is dependent on the endocannabinoid type, the receptor type, and where the receptor is located in the body. Additionally, the efficacy differs between the two endocannabinoids. 2-AG binds well to both CB1 and CB2 receptors, while AEA has low affinity for CB1 receptors and even lower for CB2 receptors (6, 16).
Metabolic Enzymes
The third component of the endocannabinoid system is enzymes. The role of these enzymes is to quickly destroy endocannabinoids once they are done with their task (10). The two main enzymes involved are called FAAH (fatty acid amide hydrolase) and MAGL (monoacylglycerol lipase). FAAH breaks down AEA, while MAGL and FAAH both break down 2-AG (17). Their job is to make sure that the endocannabinoids get used when they are needed, but not for any longer. This quick destruction is a unique process that does not occur with other molecules in the body. Because cannabinoids are quickly synthesized and destroyed, fewer long-term side effects are created (10).
More on the Endocannabinoid System
The endocannabinoid system seems to only engage when it’s needed to obtain homeostasis, and not otherwise. Research so far has shown that this system regulates various central neural activities (3) like brain firing (8), inflammation (1), anxiety, depression (3), digestion, metabolism, chronic pain, mood, memory, liver function, and much more (9).
Inflammation in particular has been studied as it relates to the endocannabinoid system. The immune system responds to physical damage or infection with inflammation, by sending cells to the affected area to remove damaged tissue or germs. Some diseases involve chronic inflammation, or autoimmunity which is when the cells cause inflammation in the wrong part of the body. Research shows that endocannabinoids appear to be produced by the immune system response, and help aid with anti-inflammation. Therefore, manipulating the levels of endocannabinoid production may be useful in the treatment of inflammatory diseases (8).
Every human possesses a different “endocannabinoid tone”, which essentially refers to how well the endocannabinoid system is working. Some researchers believe in a theory called CECD, or clinical endocannabinoid deficiency. This theory states that dysfunctional endocannabinoid systems or low endocannabinoid tones may contribute to conditions like migraines or IBS (9). Initial research has found evidence of different AEA levels in patients with migraines, as well as evidence of endocannabinoid system dysfunction in patients with PTSD. Additionally, cannabinoids have been found to help treat some of the associated symptoms (14).
What does this have to do with Cannabis?

Cannabinoids are the same thing as endocannabinoids, but are produced by cannabis plants as opposed to the body. When cannabis is consumed, the cannabinoids bind to receptors in the brain and body just like endocannabinoids, which is why effects from cannabis occur (9).
THC is the cannabinoid that has psychoactive effects, causing a ‘high’ feeling when consumed. THC activates the CB1 receptors in the brain, causing the brain to produce a sensation of being ‘high’ (8). Although endocannabinoids also bind with the CB1 receptor, psychoactive effects are not produced by endocannabinoids. This is because they don’t interact with CB1 receptors in the same way as THC, but also because the metabolic enzymes don’t quickly break down THC like they do with endocannabinoids, so THC lingers (8). In addition to being used recreationally, studies have found THC to help mitigate symptoms of various illnesses such as anorexia and vomiting caused by chemotherapy treatment (3).
CBD is the other popular cannabinoid found in cannabis. Unlike THC, CBD does not cause psychoactive effects when consumed. Initial research does show that CBD may aid with some health issues, which is why it’s being studied and consumed. CBD doesn’t appear to activate CB1 or CB2, but instead interacts with other unknown receptors (3, 9). It is also unique in that it affects overall levels of endocannabinoids in the brain, or the endocannabinoid tone (8). Research shows that CBD inhibits the FAAH enzyme which prevents it from breaking down AEA. Since increased AEA levels have been shown to treat anxiety, this may be why CBD has also been linked with anxiety reduction (8). Several studies have shown CBD to help with chronic pain (3).
It has also been found that a terpene called β-caryophyllene selectively targets the CB2 receptor (10). Studies have shown this terpene to have anti-inflammation and pain relief properties. Further research is exploring this concept as a treatment option for multiple sclerosis (13).
Hydroxylation
When THC (Delta-9-THC) is consumed, it undergoes a hydroxylation reaction. This process differs depending on what method is used to consume the cannabis. When edibles are consumed, THC enters the liver and is metabolized. This process turns most of the Delta-9 into 11-Hydroxy-THC. This 11-Hydroxy is much smaller than the Delta-9, so it has an easier time penetrating the brain. It also binds more efficiently to CB1 receptors. This is why edibles cause a more intense psychoactive effect, as well as lasting longer (2).
If inhaled, THC enters the bloodstream and circulates the body. During this circulation, some of it is metabolized into a small amount of 11-Hydroxy-THC. Then, both the Delta-9 and the 11-Hydroxy penetrate vascular tissue like the brain and muscles. When cannabis is consumed sublingually, meaning under the tongue, it dissolves and penetrates the glands and mucus membrane. THC enters the bloodstream this way and the rest of the process is the same as the inhalation process (2).
Entourage Effect
Cannabis researchers are exploring a theory called the entourage effect, which posits that multiple cannabinoids and terpenes consumed in conjunction may enhance each other’s effects. This theory came about in 1998 when two professors suggested that some inactive molecules caused an increase in endocannabinoid activity. This inspired a line of research to confirm that botanical drugs may be more effective than isolates. In the pharmaceutical industry, isolates are used for treatments, however more research is beginning to show evidence of “botanical synergy.” In cannabis, this means that other cannabinoids and terpenes in addition to THC may contribute to the overall effect (4).
One study found that a cannabis extract containing small amounts of THCA (THC in its raw state) and another cannabinoid called CBG was more effective in treating breast cancer cells than pure THC. Another study looking at epilepsy found that 71% of patients improved after using CBD-dominant cannabis extract, as opposed to 36% of patients improving from pure CBD (4).
Even though CBD doesn’t appear to interact with the CB1 or CB2 receptors, studies are finding that it seems to have an indirect effect on cannabinoid receptors, enhancing the effects of THC (3). This finding has also been confirmed anecdotally. A common report from recreational cannabis users is that CBD mitigates some of the negative effects caused by THC such as anxiety and paranoia (18). There are many other cannabinoids and terpenes that may be involved in this effect, but more research will need to be done.
Conclusion
It is pretty remarkable that human bodies produce their own cannabinoids, and therefore have a system in place that can utilize the cannabinoids found in cannabis. In fact, all vertebrate animals possess the endocannabinoid system, which is why some people are experimenting with using cannabis products to treat ailments in their pets as well as themselves. As research continues to grow around the subject, more will be understood about what the various cannabinoids are, what they do, and how they can be used to treat symptoms and diseases.
Citations
1) De Laurentiis, A., Araujo, H. A., & Rettori, V. (2014). Role of the endocannabinoid system in the neuroendocrine responses to inflammation. Current pharmaceutical design, 20(29), 4697–4706. https://doi.org/10.2174/1381612820666140130212957
2) Cannabis Science. (2019, May 31). Science You Can Eat – How and Why Edibles Work (and Sometimes Don’t). Periodic Edibles. Retrieved from https://www.periodicedibles.com/blog/science-of-edibles
3) Zou, S., & Kumar, U. (2018). Cannabinoid Receptors and the Endocannabinoid System: Signaling and Function in the Central Nervous System. International journal of molecular sciences, 19(3), 833. https://doi.org/10.3390/ijms19030833
4) Russo E. B. (2019). The Case for the Entourage Effect and Conventional Breeding of Clinical Cannabis: No “Strain,” No Gain. Frontiers in plant science, 9, 1969. https://doi.org/10.3389/fpls.2018.01969
5) Bennett, P. (2019, April 17). Meet the ‘bliss molecule’ Anandamide, a cannabinoid your body produces. Leafly. Retrieved from https://www.leafly.com/news/science-tech/meet-bliss-molecule-anandamide-cannabinoid
6) Lu, H. C., & Mackie, K. (2016). An Introduction to the Endogenous Cannabinoid System. Biological psychiatry, 79(7), 516–525. https://doi.org/10.1016/j.biopsych.2015.07.028
7) Ueda, N., Tsuboi, K. & Uyama, T. (2015). Metabolic enzymes for endocannabinoids and endocannabinoid-like mediators. In Di Marzo, V. & Wang, J. (Eds.), The endocannabinoidome: The world of endocannabinoids and related mediators. (111-135). Academic Press. Retrieved from https://www.sciencedirect.com/science/article/pii/B9780124201262000080
8) Jikomes, N. (2016, December 12). What is the endocannabinoid system and what is its role? Leafly. Retrieved from https://www.leafly.com/news/science-tech/what-is-the-endocannabinoid-system
9) Raypole, C. (2019). A simple guide to the endocannabinoid system. Healthline. Retrieved from https://www.healthline.com/health/endocannabinoid-system
10) Sallaberry, C. A. & Astern, L. (2018, June 1). The endocannabinoid system, our universal regulator. Journal of Young Investigators. Retrieved from https://www.jyi.org/2018-june/2018/6/1/the-endocannabinoid-system-our-universal-regulator
11) Mackie, K. (2008, April 17). Cannabinoids receptors: Where they are and what they do. Journal of Neuroendocrinology. https://doi.org/10.1111/j.1365-2826.2008.01671.x
12) Rogers, K. (2019, February 7). G protein-coupled receptor. Encyclopaedia Britannica. Retrieved from https://www.britannica.com/science/G-protein-coupled-receptor
13) Alberti, T. B., Barbosa, W. L., Vieira, J. L., Raposo, N. R., & Dutra, R. C. (2017). (-)-β-Caryophyllene, a CB2 Receptor-Selective Phytocannabinoid, Suppresses Motor Paralysis and Neuroinflammation in a Murine Model of Multiple Sclerosis. International journal of molecular sciences, 18(4), 691. https://doi.org/10.3390/ijms18040691
14) Russo E. B. (2016). Clinical Endocannabinoid Deficiency Reconsidered: Current Research Supports the Theory in Migraine, Fibromyalgia, Irritable Bowel, and Other Treatment-Resistant Syndromes. Cannabis and cannabinoid research, 1(1), 154–165. https://doi.org/10.1089/can.2016.0009
15) Schöneberg, T., Schulz, A., Biebermann, H., Hermsdorf, T., Römpler, H., & Sangkuhl, K. (2004). Mutant G-protein-coupled receptors as a cause of human diseases. Pharmacology & therapeutics, 104(3), 173–206. https://doi.org/10.1016/j.pharmthera.2004.08.008
16) Reggio P. H. (2010). Endocannabinoid binding to the cannabinoid receptors: what is known and what remains unknown. Current medicinal chemistry, 17(14), 1468–1486. https://doi.org/10.2174/092986710790980005
17) Basavarajappa B. S. (2007). Critical enzymes involved in endocannabinoid metabolism. Protein and peptide letters, 14(3), 237–246. https://doi.org/10.2174/092986607780090829
18) Rahn, B. (2016, July 3). Can CBD undo the anxious side effects of THC? Leafly. Retrieved from https://www.leafly.com/news/cannabis-101/can-cbd-undo-the-anxious-side-effects-of-thc
